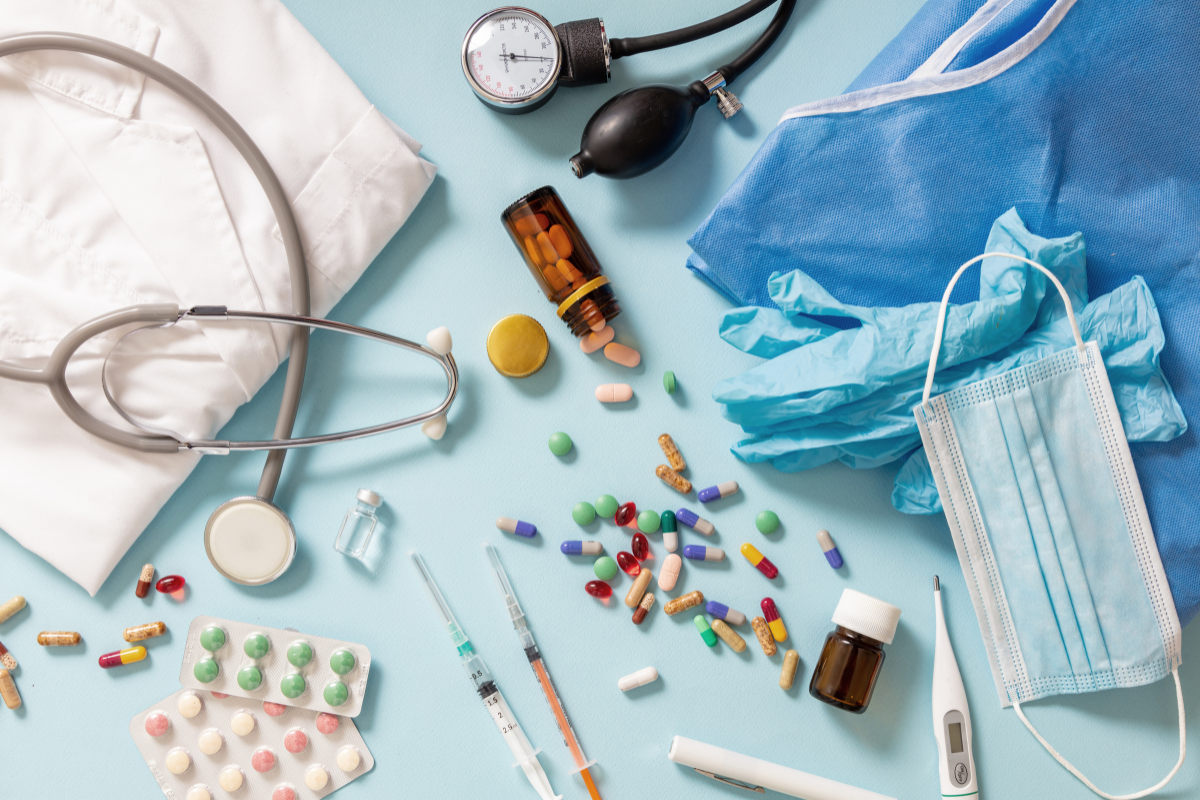
In recent years, there has been a shift away from the long-standing just-in-time inventory model in the medical supply field. The COVID-19 pandemic supply shortages highlighted this unpredictability and exposed vulnerabilities in relying heavily on a lean management system. These vulnerabilities have become clearer and are increasing with current volatility from global supply chain disruptions, transportation bottlenecks, trade tensions, and rising tariffs.
Let's explore the evolution from just-in-time inventory models to incorporating safety stock, also known as just-in-case inventory, and its role in building supply chain resilience in inventory management. This blog will also discuss how this shift is influencing medical supply strategies, emerging supply chain and technology trends, and the latest Federal Food, Drug, and Cosmetic Act (FDA) regulatory changes and developments related to compounding pharmacies.
The Operational Shift From Just-in-Time to Safety Stock
As we move further into 2026, there is more emphasis than ever on incorporating safety stock to build resilience. This is due to the current supply chain volatility, which can leave companies vulnerable to severe stockouts. Rather than a complete shift away, many businesses and organizations are adopting a hybrid inventory approach for supply chain management. This combines just-in-time inventory, which helps minimize stock and reduce costs, with a just-in-case inventory system for stocking up on critical or high-risk supplies to stay prepared for the unexpected.
These are a few ways safety stock inventory models prioritize resilience:
-
Buffer Inventory: This includes maintaining national reserves for essential supplies such as syringes, sterile vials, personal protective equipment (PPE), and disposables. These reserves help prepare for critical demand spikes beyond immediate needs and for transportation and supplier delays, serving as a short-term buffer if immediate supply were unavailable or unreliable. This supports the continuity of patient care rather than the previous focus on cost efficiency, with many organizations shifting from a minimum of 14-day safety stock to 60-day or more reserves for certain critical supplies.
For laboratories and pharmacies, it has also become increasingly common practice to maintain internal contingency reserves to help protect against unpredictable demand surges and keep operations running smoothly.
-
Dual Supplier Sourcing: There is a growing strategy to diversify supply sourcing through focusing on near-shoring and increased investment in U.S.-based manufacturing facilities. This offers greater flexibility and security to help reduce dependency on single or foreign suppliers and ensure the predictability of inventory procurement. Leading researchers expect increased investment in these new production facilities, which will provide flexibility by building more resilient manufacturing capabilities.
-
Demand Forecasting: The utilization of AI-driven data analytics, market trends, and seasonal patterns enables facilities to better predict needs, adjust, and optimize inventory based on lead-time volatility. These data-driven insights work to help improve cost efficiency while allowing organizations to anticipate and predict supply and demand shifts. By using technologies such as RFID tracking, companies can gain end-to-end visibility across the supply chain. In combination with AI, this enables organizations to ensure stock levels are replenished and optimally maintained by identifying shortages before they happen.
-
Inventory Digitization: To optimize safety stock levels, in combination with demand forecasting, the use of AI forecasting and IoT-enabled technology in inventory management is rising. These tools, including RFID tags and smart sensors, track usage in real-time and automate reordering of essential supplies. The use of these tools helps ensure supplies are correct, unexpired, and untampered with, and that they are fully accounted for and utilized, reducing waste and improving efficiency, accuracy, and safety.
While safety stock has become an important addition, just-in-time inventory models continue to work well for some lower-risk supplies, reducing waste and costs where risk is low, and suppliers are reliable and predictable.
The strategic inventory approach, with the addition of safety stock, acts as an essential buffer, helping companies stay better prepared and adaptable to spikes in demand, maintain operational continuity for patient care, and minimize risks from unpredictable or volatile demand and supply chain delays.
The Emerging Trends Shaping the Medical Supply Industry
The medical supply chain is undergoing a significant restructuring and digital transformation, with changes in how products are being manufactured, distributed, and managed. Within the hybrid approach, there is an increased use of technology to support inventory management and supply chain visibility, compliance, and cost efficiency by optimizing operational performance and streamlining healthcare providers' workflows.
Some of these trends and technology integrations helping to enhance resilience against geopolitical tensions include:
-
AI Integration and Cloud-Based Platforms: The use of AI in supply chain management provides a proactive network to improve accuracy and efficiency through data-driven analytics. This data can aid in predictions in supply chain management, which is expected to increase across hospitals, pharmacies, and laboratories, to help identify inefficiencies, forecast demand, and improve inventory allocation.
There is a digital shift towards cloud-based supply chain platforms that will continue to evolve over the next few years. Leading researchers estimate that around 70% of U.S. health organizations will continue to adopt this management system through 2026 to boost productivity, strategy, and efficiency for informed decisions. These cloud-based systems help to improve the ability to track and respond more quickly to supply shortages, while reducing waste and automating procurement processes. In turn, this can minimize administrative errors and increase return on investment for companies when navigating the complexities of fragmented, global supply chains.
-
Supply Chain Resilience and Localization: This increased investment in U.S.-based manufacturing, distribution centers, and cold-storage facilities for medicines aims to combat shortages and mitigate the risk of reduced global supply.
As demand for biologics, specialty drugs, and therapies continues to rapidly increase, there has been a crucial investment in cold chain solutions. This includes the expansion of refrigerated warehouses and specialized transportation to maintain precise temperature-controlled conditions during handling, transporting, and storing sensitive biologics and medications. The need for temperature-controlled storage across a range of products has further driven this effort for localized production, which helps decrease foreign dependence and ensures product integrity and preservation.
-
Regulatory Compliance and Cost Pressures: The continuously evolving and strict FDA regulatory frameworks for manufacturers and distributors help ensure compliance and that the required standards for safety, sterility, and quality are met.
The projected rising global healthcare costs are increasing pressure on organizations to source cost-efficient medical supplies without compromising on high-quality. By partnering with reliable, localized suppliers, healthcare providers can ensure adherence to compliance standards while better managing expenses.
-
Sustainability Efforts: There is a growing effort to reduce carbon footprint for sustainability in supply chain procurement and management to minimize waste, with stricter ESG (Environmental, Social, and Governance) compliance for manufacturers. This move has required an increased use of eco-friendly, biodegradable materials for many supplies, including gloves, PPE gowns, and plastic-free packaging.
The use of AI and digital tracking for precise inventory monitoring and management can enable better control of supply usage, helping inform ethical sourcing and prevent product expiration, reducing overall medical waste.
-
Cybersecurity: Aside from building supply chain resilience, it is equally important to remain resilient against cyber threats, as these systems have become interconnected through IoT-enabled devices and cloud-based platforms. A digital breach of data could cause severe disruption to the continuity of care and trigger stockouts. To mitigate this risk in 2026, there is an increase in Zero Trust Architecture (ZTA) for medical procurement, requiring strict identity verification for every user and device.
By investing in these technology integrations, digital inventory management platforms, and automation tools, healthcare organizations can keep up with the evolving supply chain networks to remain resilient and competitive, maintaining operational stability and ensuring consistent access to essential medical supplies.
FDA Shifts on Compounding Pharmacy Regulations
There have been significant changes in compounding pharmacy production with manufacturers facing strict and evolving FDA regulatory requirements within ongoing shifts through 2025/2026. This regards mainly ingredient sourcing and the marketing of products from compounding pharmacies that are close copies of popular medications, which have had significant demand increases in recent years.
-
The GLP-1 and ‘’Mass Compounding’’ Crackdown:
Under the proposed Safeguarding Americans from Fraudulent and Experimental (SAFE) Drugs Act, there has been a focus on non-FDA-approved compounded GLP-1 receptor agonist medications (Semaglutide and Tirzepatide). This has targeted the ‘’copycat’’ products under the FD&C Act enforced by the FDA, similar to Wegovy and Zepbound, as well as misleading advertising and the use of unsafe, unapproved Active Pharmaceutical Ingredients (APIs).
It would introduce a federal reporting requirement and tighten oversight by including a restriction to limit 503A pharmacies from large-scale production of drugs that are ‘’essentially copies’’ of commercially available medications. This change would help ensure care is provided as intended, making changes to meet specific individual needs with recorded medical reasons, including allergies, dosage form changes, and strength adjustments, rather than unregulated production.
It would also limit 503B outsourcing facilities from producing large volumes of drugs not on the FDA shortage list. For example, as certain GLP-1 medications were moved off the FDA drug shortage list, the discretionary period for mass-compounding production of this drug in 2025 ended. This marked a move to curb the sale of compounded GLP-1s.
-
Monitoring of API Sourcing
In 2025/2026, there has been an increased scrutiny of API sourcing and introduction of approved ingredients, often referred to as a ‘’green list’ to monitor this. This is part of an effort to block unapproved, foreign-sourced, or unverified APIs from the US market. As well as a move to control the mass marketing of compounded drugs that are copies of a range of approved, commercially available drug products. These changes aim to protect patients from potentially harmful mass-compounded drugs and to limit production quantities unless tailored to an individual patient with specific medical needs when FDA-approved drugs are unavailable or unsuitable.
-
The Enforcement of the Drug Supply Chain Security Act (DSCSA)
In November 2025, the deadline for the Drug Supply Chain Security Act (DSCSA) and the full enforcement came into effect, ensuring prescription drugs are verified through a comprehensive, serialized, and secure electronic tracking system. This was designed to improve end-to-end transparency across the pharmaceutical supply chain.
The policies of the DSCSA include:
-
Enhanced Verification Procedures
-
Product Serialization for Identification
-
Interoperable Data Systems
-
Product Tracing for Improved Recall and Investigation
This is all part of an effort to enhance compliance and security to prevent the circulation of counterfeit or contaminated products across all dispensers. For smaller dispensers with around 25 or fewer employees, some exemptions are extended until November 27, 2026, to meet the full requirements.
These regulatory changes over 2025-2026 include stricter reporting obligations to increase the oversight of ingredient sourcing and monitor the marketing practices being used by these compounding pharmacies.
Strategies to Meet Regulatory Compliance Standards
In 2026, the FDA issued 30 warning letters to pharmaceutical and telehealth firms over false and misleading advertisement claims that compounded products contain the same active ingredients or are equivalent to FDA-approved generic versions of branded drugs. Along with cease-and-desist letters, this has led to increased litigation with the potential for product seizure.
To ensure compliance, it is recommended to follow strategies, including:
-
Strengthen Documentation: To support clinical justification for all compounded products, maintain detailed records of procedures, ingredient sourcing, and patient prescriptions for regulatory inspections.
-
Conduct Regulatory Gap Analysis: To keep up to date on FDA requirements and state-specific regulations to ensure current pharmacy practices meet the latest standards.
-
Evaluate Operations and Monitor Litigation: By reviewing internal processes and staying aware of FDA shifts and enforcement actions, it can help identify and address gaps to adjust practices and avoid common pitfalls before they lead to compliance issues.
For 2026, the role of compounding pharmacies in creating customized medications for individuals with long-term health conditions is expected to continue to expand. This growth is driven by increasing demand for treatments that require flexibility, such as hormone replacement therapy (HRT), pain management, and geriatric care. By following these strategies and adopting new technologies, compounding pharmacies can reduce regulatory risk, maintain compliance amid shifting FDA standards, and deliver consistent quality and safety for greater patient care.
Preparing for Supply Chain Volatility and Building Resilience
For healthcare providers, laboratories, and pharmacies, building supply chain resilience is essential to handle fluctuating demands, product diversity, and regulatory requirements. This is where connecting with a trusted supply partner, not only to help manage procurement but to ensure shorter lead times and quality assurance for the supplies you source, is crucial.
As you continue to plan and navigate the evolving supply chain landscape, prioritizing long-term stability over short-term efficiency and staying up to date on smart inventory tools helps build lasting resilience, maintain operational continuity, and deliver consistent patient care.
For many years, Med Lab Supply has proudly been a reliable, trusted source of high-quality medical supplies. We have made it a priority to put the safety of our customers first and make it our mission to stock critical items that help ensure you stay operational and maintain compliance, including:
-
Sterile Syringes and Needles
-
PPE Gear (Surgical Gloves, Masks, and Gowns)
-
Disinfectants for Infection Control
-
Wound Care
-
Sterile Vials and Closures
Visit Med Lab Supply today to explore our full range of supplies and stock up with quick delivery and bulk ordering options to stay better prepared against disruptions in 2026 and beyond.